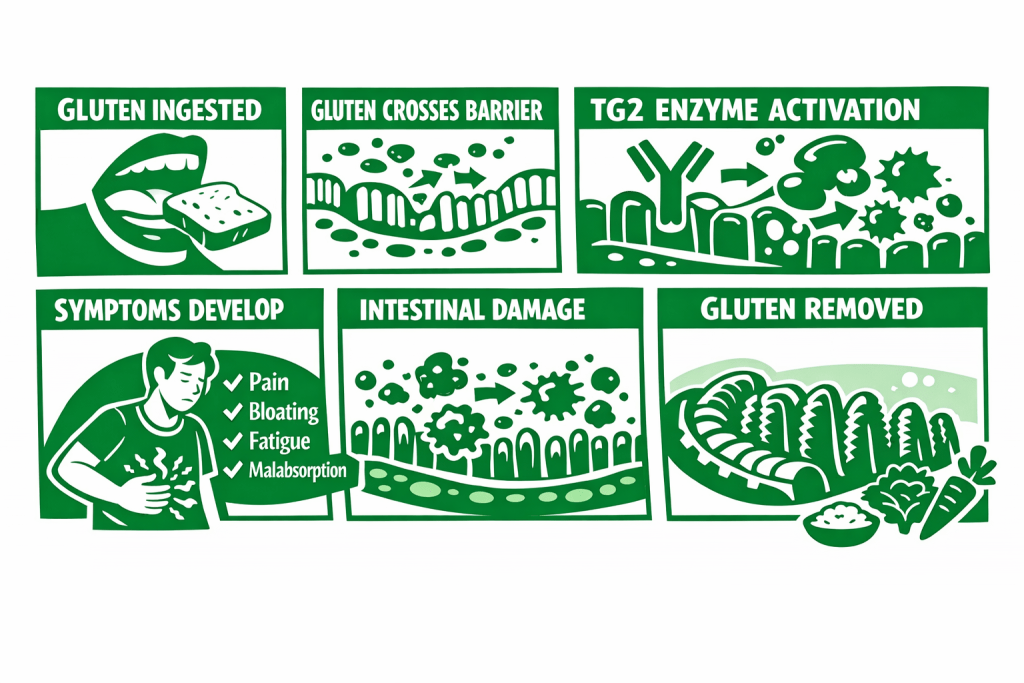
Before we talk about experimental drugs, nanoparticles, immune tolerance, and all the cool science coming down the pipeline, we need to start with the basics.
What actually happens in the body when someone with celiac disease eats gluten?
Because it’s not just “gluten hurts the gut.”
It’s a multi-step immune reaction.
Let’s walk through the journey of one tiny crumb of gluten.
Step 1: Gluten enters the digestive system
Gluten is a protein found in wheat, barley, and rye.
When most people digest gluten, enzymes break it down into smaller pieces.
But gluten has a problem:
Some fragments are very resistant to digestion.
One of the most famous fragments is a 33-amino-acid peptide that survives stomach and intestinal digestion.
So instead of being fully broken down, pieces of gluten reach the small intestine mostly intact.
Step 2: Gluten crosses the intestinal barrier
Normally, the intestinal lining acts like a tight security gate.
But gluten fragments can cross the lining through:
• tiny gaps between cells
• immune sampling cells in the gut
• inflammation that loosens the barrier
Once those fragments cross the lining, they enter the immune system’s territory.
And that’s when the real trouble begins.
Step 3: The TG2 enzyme modifies gluten
Inside the intestinal tissue lives an enzyme called:
Tissue transglutaminase (TG2)
TG2 modifies gluten peptides in a process called deamidation.
That modification makes gluten much more visible to the immune system in people with certain genes.
This is the step that turns gluten from food into a target.
(And it’s why some of the newest celiac drugs try to block TG2 entirely.)
Step 4: Genetic risk turns on the immune response
Almost everyone with celiac disease carries one of two genetic markers:
• HLA-DQ2
• HLA-DQ8
These molecules sit on immune cells and present gluten fragments to T-cells.
When TG2-modified gluten binds to these molecules, it triggers gluten-specific T-cells.
Those T-cells then release inflammatory signals.
The immune system now believes gluten is dangerous.
Step 5: The intestinal lining becomes collateral damage
Once the immune response starts, several things happen:
• inflammatory cytokines are released
• immune cells infiltrate the intestinal lining
• epithelial cells are attacked
This leads to villous atrophy.
Those tiny finger-like projections in the intestine (villi) flatten.
When that happens, the intestine loses surface area needed to absorb nutrients.
Step 6: Symptoms appear
The symptoms of celiac disease come from two places:
1️⃣ Inflammation
This can cause:
• abdominal pain
• bloating
• diarrhea
• nausea
• fatigue
2️⃣ Malabsorption
Because damaged villi can’t absorb nutrients properly.
This can lead to:
• anemia
• weight loss
• vitamin deficiencies
• neurological symptoms
• bone loss
And some people experience almost no digestive symptoms at all, which makes diagnosis tricky.
Step 7: Removing gluten stops the immune attack
When gluten is removed from the diet:
• the immune trigger disappears
• inflammation gradually decreases
• the intestinal lining begins to heal
In children, the intestine may heal within months.
In adults it often takes 1–2 years for full recovery.
But here’s the important part:
The immune system never forgets gluten.
Even after years on a strict gluten-free diet, a tiny exposure can restart the entire cascade.
The question scientists are trying to answer now
Most current treatments focus on avoiding gluten entirely.
But researchers are asking bigger questions:
• Can we block the TG2 step?
• Can we digest gluten before it triggers immunity?
• Can we teach the immune system to tolerate gluten again?
Those ideas are exactly what current clinical trials are trying to solve.
And that’s where Science Wednesday is going next.
Next week we’ll talk about something wild:
Scientists are trying to retrain the immune system using nanoparticles filled with gluten.
Yes.
On purpose.
And early trials suggest it might actually work.
Before we dive deeper into the science next week:
What symptom tipped you off that something wasn’t right before your diagnosis?